
I often hear pediatric dentists pondering the following question. When is the right time to invest in an all-issue dental laser? For some the right time never comes. For others, it’s as soon as possible. The answer to this dilemma is really quite simple, depending on how you respond to the following questions. Do you want to be a tooth-o-dontist? Are you satisfied to just “drill and fill?” Or, do you want to be a physician of the oral cavity?
As dentistry and medicine merge closer together, the pediatric dentist should be in the forefront of understanding how the oral structures—teeth, jaws, and especially the tongue—can impact many of the body’s systems.1 Normal jaw and tongue positions are critical to maintaining a good patent airway for infants and toddlers as well as older children. Being a practitioner who just maintains the integrity of teeth is no longer adequate.
We also need to understand how we are in the best position to diagnose obstructive sleep apnea or sleep-disordered breathing in newborns, infants and toddlers. In addition, we must be aware of how dental infections may affect our patients’ overall health, their total growth, and their development. Tethered oral tissues (TOTS) such as the upper lip-tie and lingual ties may restrict the entire body due to the involvement of the body’s fascial system. 2 Our practices need to see infants as soon as possible when mothers suffer a plethora of different breastfeeding problems related to these tethered oral tissues.
As pediatric dentists, we wear many hats. We may assist mothers that stress over failing to successfully breastfeed their infants and often suffer from post-partum depression, fail to successfully bond with their infants, and end up using bottles and formula. Infants with ankyloglossia (tongue-tie) may suffer from reduced oxygen flow due to blocked airways. This in turn can directly affect the respiratory and circulatory systems.3,4 Studies now indicate that ankyloglossia may also be related to infant’s developing ADD/ADHD in the future. Infants who have a restricted tongue may fail to latch securely to their mother’s breast and swallow large amounts of air, resulting in air-induced reflux, which in turn is treated with drugs by the medical profession.
We as pediatric dentists are in a position both to diagnose and help alleviate these types of conditions. Furthermore, by using an all-issue dental laser right in your own dental office, you may easily and safely correct many infant problems referenced in this article.
MAKING THE DECISION TO INVEST IN A LASER (WHAT OPTIONS ARE AVAILABLE?)
First, we need to look at the benefits of laser dentistry and determine which laser is best for you as a pediatric dentist. There are three types of lasers a pediatric dentist should be familiar with. 4 In addition, you must ask yourself several questions when making your decision. What do I want to be able to do with lasers? Am I looking to do all types of dentistry—restorative, surgical, and trauma treatment? Do I want to reduce the need for local anesthetics? Or do I perhaps only want to use lasers for soft-tissue surgery?
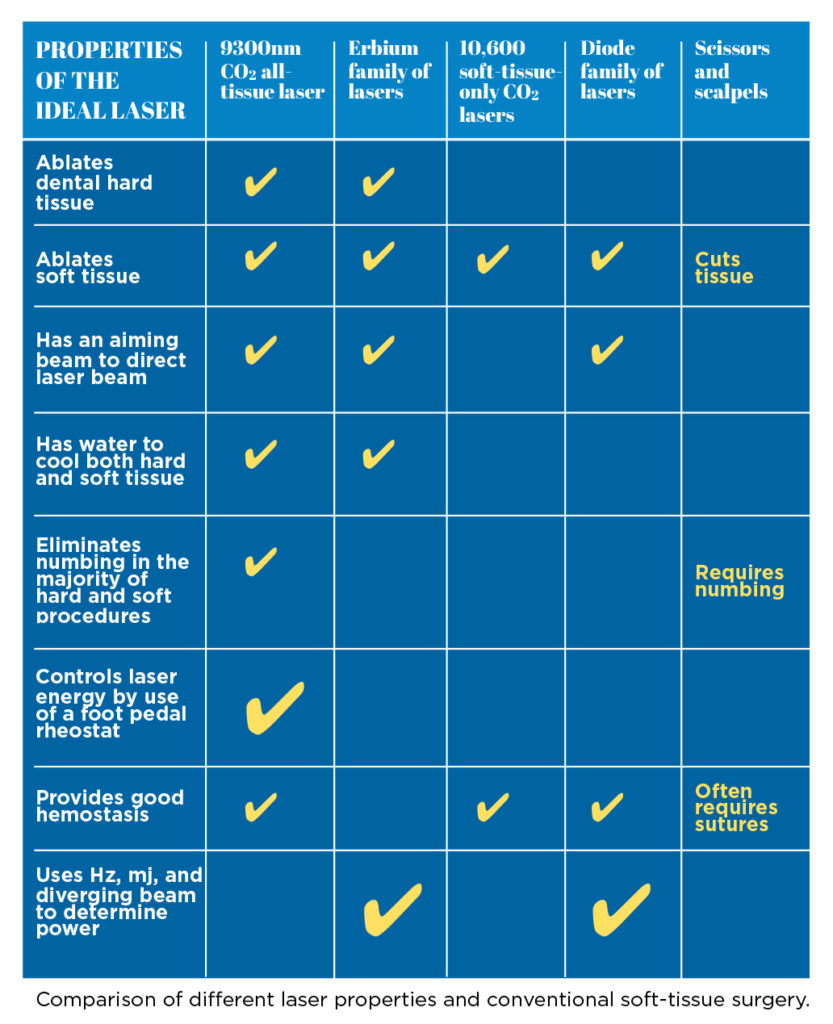
LASER CATEGORIES AND WAVELENGTH
Lasers are classified in one of two categories: 1) hot or cutting lasers, and 2) cold or non-cutting lasers. Hot lasers are lasers used to ablate hard and soft tissue and may be further classified either as all-tissue lasers or lasers limited to soft tissue surgery. Cold lasers are used in laser pointers as well as for cavity detection, treating trauma, and in certain non-ablation, soft-tissue treatment.
In general, lasers have specific target tissues or chromophores. The ability of a tissue to absorb a specific laser is determined by the laser’s wavelength, expressed in nanometers.
PHOTOBIOSTIMULATING LASERS
The first type of laser to consider would be a photobiostimulating laser (a PBM—formerly called a low-level laser). In the practice of dentistry, these lasers cannot incise or excise tissue, but a PBM may be used to reduce the effects of traumatic injuries by decreasing swelling, improving healing, treating aphthous ulcers (canker sores), aborting herpes labialis, and lowering the need for local anesthetics.5 All lasers can produce these effects depending on the power used.
SOFT-TISSUE-ONLY LASERS
The second type of laser is used for procedures involving treatment of soft tissue only. These lasers belong to either a diode family of lasers with a range of 400nm–1064nm wavelengths or soft-tissue carbon dioxide lasers limited to 10600nm wavelength only.
ALL-TISSUE LASERS
The third type includes an all-tissue laser of the erbium family of lasers and the 9300nm carbon dioxide laser. These lasers are capable of ablating enamel, dentin, and bone. They may be used in all types of soft-tissue surgery.
When asked about the negatives of investing in a laser, cost is always brought up as a major negative. This objection, however, is like a lot of “false news.” Once a dentist decides to move forward and chooses the right laser for his or her practice, the return on this investment more than covers the expense and ultimately results in improved patient care. Of course, this assumes that the dentist has received correct training in the use of lasers and has an adequate knowledge of laser physics and laser safety.
I believe we have reached what businesses call the tipping point in laser dental care. The question is no longer if, but when should you invest in a laser. The pediatric dentist who does not use an all-tissue laser will soon find patients seeking out one who does.
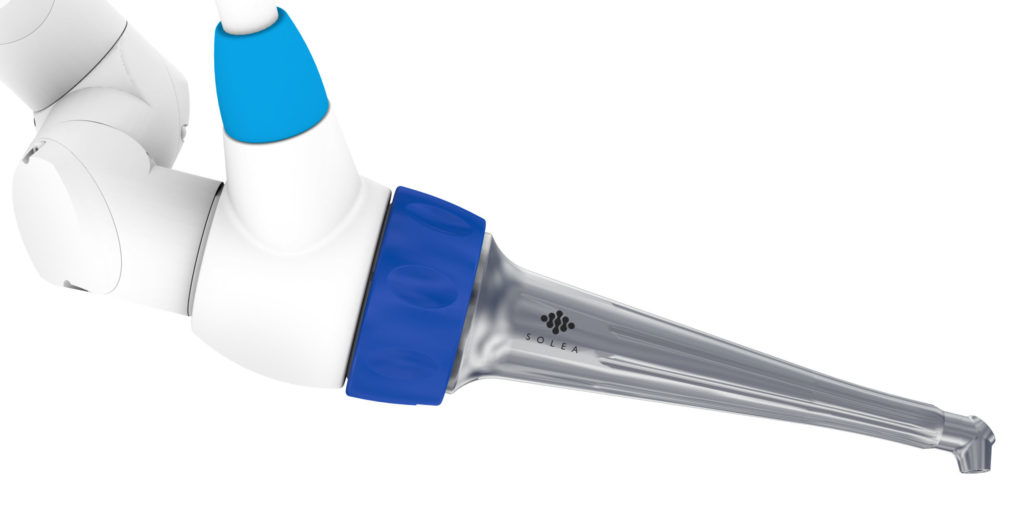
THE 9300NM ALL-TISSUE CARBON DIOXIDE LASER
Having invested in lasers since 1998, I have used a variety of equipment. Lasers I have used include an Nd:YAG (not discussed here since it is not really a laser for the pediatric dentist), erbium lasers by various manufacturers, many different diode lasers with various wavelengths, and now the 9300nm, all-tissue carbon dioxide laser. In addition to personally using many types and brands of lasers, I have lectured and taught for many of the laser manufacturers.
Based on my own experience, I have found the Solea 9300nm all-tissue laser developed by Convergent Dental to be the best. 6 Among Solea’s major differences and benefits are the following. It incorporates all the benefits of hard and soft-tissue lasers into a single unit featuring a user friendly, computer-touch-screen control panel. Solea is also the only laser using a variable foot pedal or rheostat to control laser power rather than simply employing an on-off switch. Controlling laser energy and power with this laser is similar to driving a car—you control these parameters by watching what is occurring to the tissue being treated and control ablation by controlling foot pedal pressure.
Computers control Solea’s beam size, so there is no need to change tips or handpieces during restorative or surgical treatment. All controls are fingertip controlled by the touch screen. The laser produces a safe, diode-green, laser-focus beam and allows precise water and air control during soft tissue excisions when desired.
KEEP MOST DENTAL PROCEDURES IN YOUR OWN OFFICE
Referring most soft-tissue procedures to other specialists is a thing of the past. With the exception of third-molar and other bony impactions, most soft-tissue surgery can be completed by the pediatric dentist using the 9300nm laser. Keeping all the procedures you historically referred out in your own office will more than cover your laser’s initial cost and help you realize a rapid return on your investment.
Getting the most from your laser investment, however, requires that you become educated in laser physics, laser safety, and how to optimally maintain your laser, before treating patients. A good laser manufacturer will provide in office demonstrations and an in-depth introduction to their laser’s capabilities. This introduction will include information on the laser’s specific settings and parameters as well as instruction in using the laser to perform specific procedures which it was designed to accomplish.
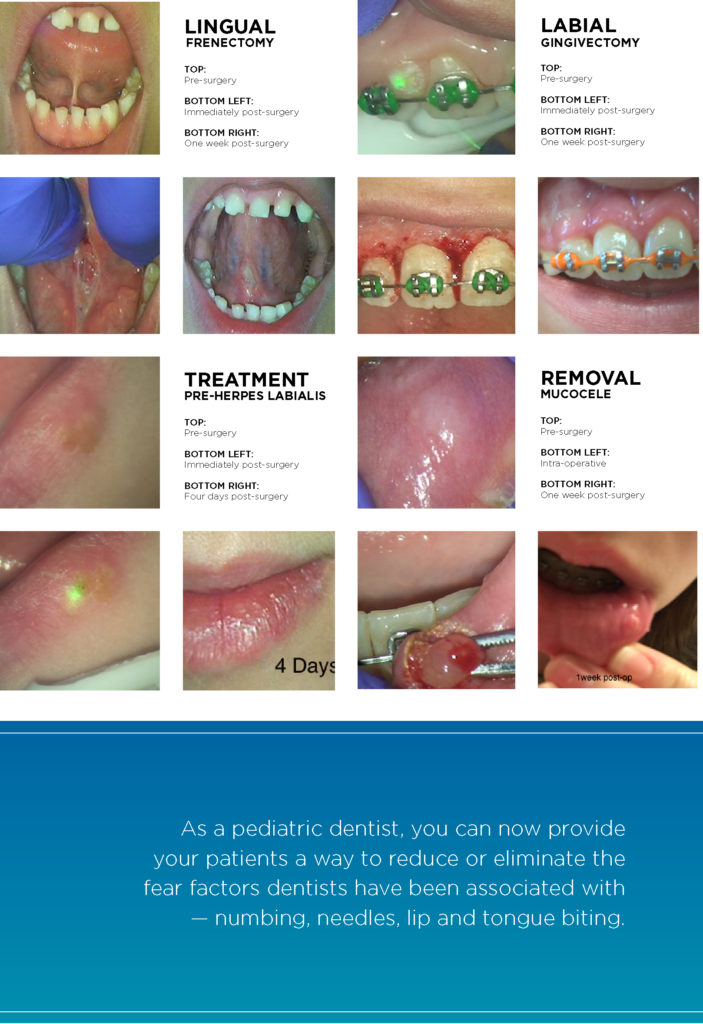
As a pediatric dentist, you can now provide your patients a way to reduce or eliminate the fear factors dentists have been associated with—numbing, needles, lip and tongue biting.
OPERATIVE DENTISTRY WITHOUT ANESTHESIA
All types of restorative dentistry—Class I-VI, anterior and posterior pediatric crowns and pulpotomies—can be completed in most patients without the need for local anesthetics. Tooth isolation using the Isolite method and a rubber dam may be accomplished using lasers to enhance treatment and care.
Benefits of using lasers (Depending on wavelength and target tissue)
- Reduces the need for local anesthetics
- Eliminates the potential for infections (lasers are bactericidal)
- Allows more restorative treatment per visit (2-4 quadrant dentistry)
- Reduces time away from school (for children receiving dental care)
- Reduces time away from work (for parents who accompany their children)
- Reduces fear factors associate with dental care
- Eliminates post-treatment emergencies and concerns about biting cheeks, lips or tongues
- Reduces stress for patients, parents, staff and dentist
- Reduces sedation and the need for general anesthesia
- Serves as an excellent practice builder
- Remains safe to use (when proper eye protection is used for everyone in the surgical area)
Negatives of using lasers
- Potential issues caused by improper or insufficient training
- Perceived high cost of investment
Soft-Tissue Procedures Pediatric Dentists May Safely Treat in the Office
- Lingual Frenectomies
- Mandibular frenotomies
- Upper lip-ties
- Hemangioma removal
- Mucocele removal
- Other biopsies
- Fibroma Removal
- Exposing teeth under bone or soft tissue
- Gingivectomies
- Phase-three orthodontics (recontouring gingical hyperplasia)
- Treatment of apthous ulcers
- Treatment of herpes labials
- Removal of venous lake lesions
- Removal of fractured root tips
- Treatment of pericoronial tissue on erupting molars
- Exposing decay on partially erupted teeth/removing excess tissues grown into decay
FINAL THOUGHTS
When I first decided to invest in lasers for my patients, lasers were a new emerging technology. Today, they are no longer on the cutting-edge of pediatric dentistry. Rather, they are the standard of care which pediatric dentists should be providing for their patients. Lasers can be used in procedures involving almost every hard and soft tissue which you as a pediatric dentist may be called upon to treat in your patients. Understanding the benefits of lasers and the training which is required to use them safely should be an essential prerequisite for all dentists who treat children.
DISCLOSURE
Over the years since I began using lasers, I have consulted with the former Hoya laser and Fotona laser companies. I have produced laser teaching videos, provided continuing education courses, and received honoraria. I have also consulted with various other companies (such as Isolite, Innovation Optics, and Specialized Care) dealing with laser accessories. At the present time, I provide training for dentist’s investing in the Solea laser and speak at various meetings for Convergent Dental on the benefits of the Solea laser. When Convergent offered investment options, I purchased some shares of their stock.
References
4. Kotlow L. Lasers and pediatric dental care. Gen Dent 2008 Nov- Dec;56(7);618–27.
5. Kotlow, L. Photobiomodulating lasers and children’s dental care. J Laser Dent 2009;17(3):125–130.


