I vividly remember the first time I met Maryclaire. It was just five days after her first birthday. She was a beautiful little girl with perfect pudgy cheeks, adorable yellow locks, and a mouth full of bluish-gray teeth. She came to my office excited for her first dental visit and left with a diagnosis of Dentinogenesis Imperfecta (DI).
As I examined her mouth, I discovered that her primary teeth all had the bluish-gray discoloration that is classically found with DI. As I began explaining my findings with Maryclaire’s mother, she was shocked and extremely concerned with the diagnosis. I immediately referred her to her pediatrician for further evaluation, and her pediatrician ordered a genetic panel. The genetic panel determined that she has a spontaneous mutation that includes Osteogenesis Imperfecta (OI). However, Maryclaire has never exhibited any manifestations of OI. Her definitive diagnosis was made after genetic testing as: Dentinogenesis Type 1; Osteogenesis Imperfecta with DI, Shield Type 1.

Dentinogenesis Imperfecta causes the teeth to be discolored (most often a blue-gray or yellow-brown color) and to exhibit translucency. Maryclaire’s teeth exhibited both color variations and translucency. DI causes weakening of the teeth, which often includes rapid wear and abnormal pulp anatomy. DI can affect both primary and permanent dentitions. Treatment modalities most often involve full-coverage restorations and Maryclaire’s case exhibited the need for full coverage in all primary teeth.
Over the next 16 months, Maryclaire was medically cleared for traditional general anesthesia in an outpatient dental surgery center and had a multitude of other medical evaluations, including cardiac and hearing screenings, which were all normal.
At my office, I kept a close eye on Maryclaire and during our in-office visits, every two to three months, we charted wear on the maxillary and mandibular incisors with continuing flaking of enamel and dentin exposure. Her parents were diligent about excellent home care and optimizing fluoride supplementation. I advised against any type of electric toothbrush to protect remaining enamel since it was so weak and unpredictable. She used an extra-soft bristle toothbrush at home that seemed to remove plaque effectively and not expedite any wear on her teeth. Maryclaire never exhibited any sensitivity in her teeth and was able to eat and speak effectively. She did have a pacifier habit until her surgery date and displayed a classic class-2 occlusion with an open bite that was habit related.
I created a treatment plan based on her clinical and radiographic findings. This plan included full-coverage crowns on all 20 deciduous teeth. i had no reservations about my ability to prepare her canines and lateral incisors for zirconia crowns.
Between our first visit and her treatment date, all of her primary teeth erupted fully and all exhibited DI. We were able to obtain radiographs prior to her general anesthesia date and were able to assess pulpal status and size. Her incisors and canines exhibited a smaller, receding pulp chamber. Her molars exhibited larger pulp chambers with a thin enamel/dentin layer. At this point, my main concern was the size of the molar pulps and exactly how much tooth structure would be preserved during crown preparation.
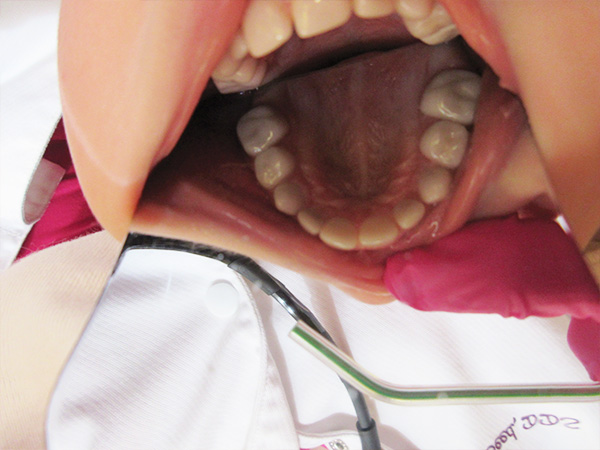
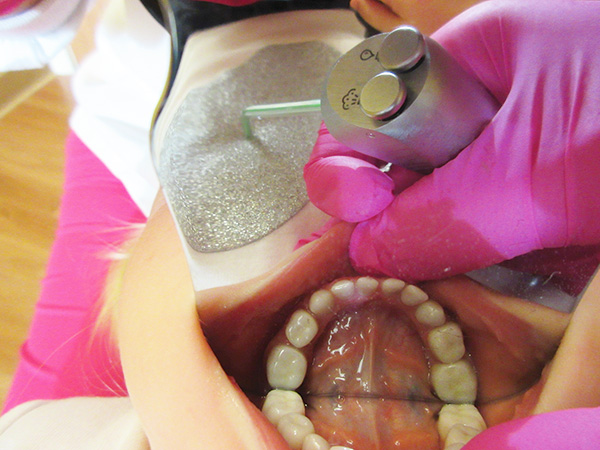
I created a treatment plan based on her clinical and radiographic findings. This plan included full-coverage crowns on all 20 deciduous teeth. I had no reservations about my ability to prepare her canines and lateral incisors for Zirconia crowns. However, I tentatively planned on placing stainless steel crowns on her molars to reduce the risk of pulpal exposure. I reviewed with her parents that the most important aspect of placing crowns for her would be to avoid pulpal exposure since her pulp chambers were abnormally shaped and might not respond predictably to pulpal treatment. I did let them know that once I started preparation there was a small chance that I could place Zirconia crowns on her molars as well.
Due to deterioration and loss of enamel on her anterior teeth, I elected to do treatment under general anesthesia when she was two years and four months of age. She responded well under general anesthesia, and we completed all her restorations in one visit. She even stopped her pacifier habit and potty trained herself in the week following treatment!
During treatment, I prepared her incisors and canines first and cemented her crowns in groups of two to three to simplify alignment, ensure hemostasis, and to be able to apply finger pressure to each tooth as the cement hardened. I used Ketac cement for all crowns.
Her anterior preparations were classic and straightforward with no signs of nearing her pulp chambers. As I approached her posterior molars, I prepared the occlusal surfaces first and was anxious about what amount of pulpal tissue I might encounter as I prepared the teeth. However, I was able to perform enough occlusal reduction for Zirconia crowns with no sign of a blushing pulp. The rest of the molar preparation was conservative, and I had no problem preparing the mesial-distal-buccal-lingual surfaces without nearing the pulp. I was extremely excited to be able to place Zirconia crowns on all of Maryclaire’s teeth!
During her treatment, clinically I was very pleased with the amount of tooth structure I was able to preserve. I wasn’t sure what quality of tooth structure I would encounter and with good reason. She had islands of remaining enamel over moderately soft to very flaky blue- gray and yellow-brown dentin underneath. I prepared the teeth while removing as little tooth structure as possible and in some areas I was able to preserve a moderate amount of enamel.
Immediately following anesthesia, I spoke to Maryclaire’s parents and showed them post-operative pictures. Their response was more than I could have hoped for and was a mixture of relief and happiness that Maryclaire was finished with this first chapter dealing with DI. When Maryclaire’s parents saw her new smile, their expression was priceless and one I will never forget. I explained that Maryclaire did have a pre-existing open bite from her pacifier habit which I had to replicate, but that I felt this would close nicely if she stopped her pacifier habit soon. Maryclaire hasn’t used her pacifier since. At her follow-up appointments, we found her open bite is closing nicely, as if the crowns are completely her natural tooth structure.
As a pediatric dentist that takes pride in ensuring that each patient will experience the best possible outcome, Maryclaire’s case exceeded my expectations. The transformation of a beautiful little girl with crumbling teeth that were literally on borrowed time into a confident little girl with no reservations about her smile is unbelievably rewarding. Thanks to modern dentistry, I was able to prevent pain in her teeth and mouth, as well as protect her from the social and societal ramifications of having DI in her young, formative years.
Clinically, preparation for a Zirconia crown becomes second-nature with practice and following the steps laid out by the EZPEDO team. The learning curve with Zirconia crowns isn’t steep, and once you reach a comfort level, the ability to provide high-quality, esthetic, strong restorations is invaluable to one’s practice. This case showed me the possibilities of providing a full-mouth restoration with Zirconia crowns, but more importantly, I was able to dramatically enhance a little girl’s life.


